Slides
| A. Which patients should be treated with percutaneous endovascular intervention? |
Catheter-based therapy of the femoro-popliteal tree is the most frequently performed peripheral intervention and is an accepted first-line therapy in selected patients with intermittent claudication in whom exercise treatment combined with pharmacological therapy has failed. While the degree of a patient's disability is a prime consideration, the anticipated short- and long-term clinical benefits are the major determinants of the role of catheter techniques in patients with femoro-popliteal disease. Balloon angioplasty and metallic stent implantation are major technical advances that have improved acute procedural results and increased the use of endovascular procedures in patients with more extensive, complex disease. However, the long-term efficacy of endovascular procedures in complex lesion types has not been fully defined. |
B. Indication and contraindications for peripheral vascular intervention |
• Indication • Relative contraindication • Absolute contraindication American Heart Association and TransAtlanttic Inter-Society Consensus (TASC II) document provides evidence-based recommendations for treatment to intermittent claudication patients. In TASC II, femoro-politeal lesions are classified into 4 categories: type A-D. TASC classification of femoral popliteal lesions.
• TASC A and D lesions: Endovascular therapy is the treatment of
choice for type A lesions and surgery is the treatment of choice for type
D lesions. - ACC/AHA guideline summary : endovascular treatment for claudication Class I - There is evidence and/or general agreement that endovascular
treatment is beneficial in the following settings Class IIa - The evidence or opinion is in favor of endovascular
treatment being beneficial in the following setting Class IIb - The evidence or opinion is less well established
that endovascular treatment is beneficial in the following settings Class III - There is evidence and/or general agreement that endovascular
treatment should not be performed in the following settings |
C. Is routine stenting beneficial over peripheral transluminal angioplasty (PTA) alone in terms of immediate and long-term results? |
| The technical and clinical success rate of PTA of femoropopliteal artery stenoses in all series exceeds 95% (range 98%–100%, standard error 1.0%).1 Device developments such as hydrophilic guide wires and technical developments, such as subintimal recanalization, provide high recanalization rates in total occlusions of more than 85% (range 81%–94%, standard error 2.9%).2 The technique of subintimal angioplasty is not as dependent on length, but rather on the presence of normal vessel above and below the occlusion to allow access.3 Stents have been designed to improve the technical success rate and overall arterial patency after peripheral transluminal angioplasty (PTA). By fixing arterial plaque against the arterial tree, stents prevent immediately recoil and obstructive plaque dissection. However, there is a tendency for loss of initial patency due to restenosis (which usually occurs in the first six months) or to progressive atherosclerosis at the lesion site or elsewhere in the same vessel. The smaller vessel diameter is probably the major explanation for the higher rate of restenosis compared to iliac disease. Previous small randomized trials failed to demonstrate the superiority of PTA plus stent over PTA alone in the femoro-popliteal tree. The largest randomized trial.4 comparing PTA alone versus PTA plus stent (Palmaz, stainless steel stent) in the superficial femoral artery in 227 patients showed that stent use was required in 15% of the PTA-alone group; and 1-year angiographic restenosis was not statistically different between PTA alone and PTA plus stent (32.3% vs. 34.7%, p=0.85). Survival was not different between the PTA alone group and PTA plus stent at 4 years. Therefore, the use of stents was not supported by previous data. Stents may have a role in salvaging acute PTA failure or complications.5-8 Recently, patency at one year improved significantly with development of nitinol stents (ex. Smart stent, Dynalink stent, Expander stent). The several studies using Smart stent achieved one-year patency in 83%-88% of cases. The use of nitinol stents has reported 3-year patency rates of up to 76%.9,10 In nonrandomized one study comparing nitinol and stainless stent implantation for femoro-popliteal artery showed that cumulative patency rates at 6, 12, 24 months were 85%, 75%, and 69%, respectively, after nitinol stent implantation verus 78%, 54%, 34%, respectively after stainless steel stent implantation (p=0.008).11 this results suggested that primary placement of nitinol stents might be more effective than conventional balloon angioplasty. Recently, in a meta-analysis of randomized controlled trials, currently available data suggest no significant difference in the rate of TVR between PTA with provisional stenting and routine stenting for symptomatic patients with short SFPA lesions, although there is a trend for lower restenosis and a significant higher immediate technical success rate in favour of routine stenting as well as a non-significant trend towards lower TVR with the newer generation nitinol stents.12 *Pooled results of femoral popoliteal dilatation 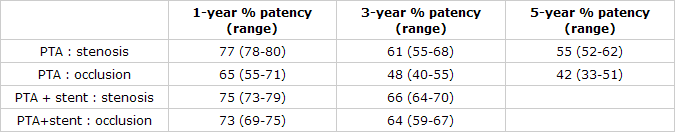 |
D. Are there any factors that affect outcomes after PTA of the femoro-popliteal artery? |
| Risk factors for recurrence were analyzed by multivariate
stepwise backward regression analyses in various studies. Clinical stage
of disease (intermittent claudication versus critical limb ischemia),
length of lesion and outflow disease were most commonly found as independent
risk factors for restenoses. Recently, a study by Schillnger of 172 patients
successfully undergoing PTA of the superficial femoral and popliteal arteries
observed that 6-month patency rates were related to hs-CRP levels at baseline
and at 48 hours after intervention.13 Anatomic factors that adversely
affect long-term patency include long or eccentric calcified lesions,
occlusion instead of stenosis, and poor distal run-off..14,15 |
E. Are there any methods for prevention of restnosis ? |
| The pathogenesis of restenosis after PTA is the same as that after coronary artery angioplasty, which smooth muscle cell proliferation and migration being the major events. A number of therapies have been tried in an attempt to prevent restenosis after femoral PTA. 1. Local delivery of paclitaxel – The THUNDER trial randomly assigned 154 patients to paclitaxel coated angioplasty balloons, uncoated balloons with paclitaxel dissolved in the contrast medium, or uncoated balloons with contrast solution containing no paclitaxel. The primary end point of mean late lumen loss after six months was significantly lower in the coated balloon group than either the paclitaxel solution or control groups (0.4 versus 2.2 and 1.7 mm, respectively). The coated balloon group also had a significantly lower rate of target lesion revascularization at six months (4 versus 29 and 37 percent).18 The findings in THUNDER were confirmed in the similarly designed FemPac trial, in which 87 patients undergoing angioplasty of femoropopliteal lesions were randomly assigned to either uncoated or paclitaxel-coated balloons catheters. The primary end point of late lumen loss at six month follow-up angiography was significantly less in the coated balloon group (0.5 versus 1.0 mm).19 2. Stenting - The composition of the stent may influence the rate of stent patency after femoropopliteal intervention and three studies have evaluated the safety and efficacy of self expanding nitinol stents compared to either PTA or steel stents. In an observation study with subsequent randomized trial showed significant reduction of restenosis in self expanding nitinol stents compared to either PTA or steel stents.20.21 But recent the FAST trial of 244 patients with a single, short (mean lesion length of 45 mm compared to 130 mm in the preceding trial) superficial femoral artery lesion and chronic limb ischemia found no advantage compared with PTA. At one year, there was no significant difference in the primary end point of binary restenosis as determined by intravascular ultrasound (32 versus 38 percent, respectively) or the secondary end points of target lesion revascularization and Rutherford category of PAD.22 3. Drug eluting stent – In SIROCCO trial, patients with chronic limb ischemia and TASC type C lesions treated with sirolimus-eluting versus bare SMART nitinol self-expandable stent, the sirolimus-eluting and the bare SMART stent are effective, safe, and free from restenosis in a majority of patients for up to 24 months. Because the restenosis rate in the bare stent group is unexpectedly low, no significant difference could be found between the sirolimus-eluting and the bare SMART stents.23 |
Reference |
| 1.G. Muradin, J. Bosch, T. Stijnen and M. Hunink,
Balloon dilation and stent implantation for treatment of femoropopliteal
arterial disease: meta-analysis, Radiology 221 (1) (2001), pp. 137?145
|


Leave a comment